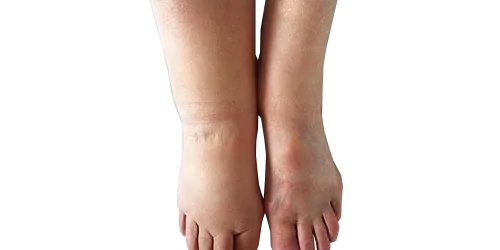
Lymphedema is a chronic swelling condition that can occur when the lymphatic system is damaged or overwhelmed – often as a side effect of cancer treatment. After enduring cancer surgery or radiation, facing lymphedema can feel like “an added insult” due to its impact on comfort and daily living. In fact, lymphedema affects roughly 1 in 1,000 people, and more than 20% of breast cancer survivors develop some degree of post-mastectomy swelling in the arm or chest . The good news is that with the right precautions and expert care, you can protect your health and quality of life. In this article, Dr. Amit Agarwal – an internationally trained plastic surgeon in Lucknow specializing in microsurgery and lymphedema management – explains the causes of lymphedema, early warning signs, practical prevention tips, and advanced treatment options (like lymphovenous bypass and lymph node transfer) available at Kayakriti Plastic Surgery. Our goal is to empower you with knowledge and confidence to manage or even prevent lymphedema progression.
Understanding Lymphedema: Causes and Risk Factors
Lymphedema is an abnormal buildup of protein-rich lymph fluid in the tissues, leading to persistent swelling of an arm, leg, or other body part. It happens when the lymphatic vessels or lymph nodes (which normally drain excess fluid and filter out toxins) are blocked, removed, or damaged. There are two main types of lymphedema:
-
Primary lymphedema: A rare, inherited or congenital condition where lymphatic vessels are malformed or reduced in number from birth. This can cause swelling to develop spontaneously (often in the legs) without any obvious trigger, sometimes emerging in adolescence or early adulthood.
-
Secondary lymphedema: A much more common form caused by an external injury to the lymphatic system. This includes cancer-related lymphedema, often seen after surgeries like mastectomy with lymph node dissection or pelvic cancer surgeries, or after radiation therapy that scars lymph nodes cancer.govcancer.gov. For example, breast cancer patients who had lymph nodes removed or radiated under the arm may later experience arm swelling (post-mastectomy lymphedema) on that side cancer.gov. Other triggers of secondary lymphedema include trauma, severe infections (such as cellulitis or filariasis in some regions), or any surgery that disrupts lymph vessels. Even years after cancer treatment, an injury or infection in the affected limb can overwhelm the reduced lymphatic capacity and lead to swelling. In fact, most lymphedema cases appear within 2-3 years of surgery, but the risk persists for life – increasing with any new trauma to that limb hse.iehse.ie. Factors like obesity and poor healing can further raise one’s risk cancer.gov.
Bottom line: If you’ve undergone cancer surgery or radiation (especially for breast, gynecologic, prostate, or melanoma), or if you have chronic vein issues or a history of serious infection, you should be aware of lymphedema. Knowing the causes and your personal risk factors will help you stay vigilant and take proactive steps to prevent arm or leg swelling after cancer surgery and other forms of lymphedema.
Recognizing Early Signs of Lymphedema
Early detection of lymphedema is crucial. In its initial stages, the signs can be subtle and easy to overlook. Common early symptoms include:
-
Unusual heaviness or tightness: You might feel a “full” or heavy sensation in the affected limb before any visible swelling appears. Some people notice that rings, watches, or sleeves feel tighter than usual on one side cancerresearchuk.orgcancer.gov. Aching or a tingling “pins and needles” sensation can also occur as fluid begins to accumulate.
-
Mild swelling that comes and goes: In the beginning, swelling may be slight and intermittent. For example, an arm or leg might appear a bit swollen at the end of the day or after exercise but returns to normal by morning. You may see a temporary dent (pitting) if you press on the area cancer.gov. These fluctuations indicate stage 1–2 lymphedema, when fluid buildup is still reversible with elevation and rest .
-
Skin changes: The skin can feel tighter or stiffer than normal. Some people notice thickened or leathery skin texture or creases appearing shallower on the affected limb. Clothing or jewelry on that limb may leave imprints due to subtle swelling. Without management, the skin can become hard and fibrous over time (a sign lymphedema is progressing) cancer.gov.
-
Reduced flexibility: You might feel limited mobility or stiffness in the nearby joints (such as shoulder tightness after lymph node dissection, or ankle stiffness with leg lymphedema). Swelling around tendons and muscles can make it harder to move the limb freely cancer.gov.
If you have had cancer treatment, it’s wise to monitor the at-risk limb during and after therapy for any of these signs cancer.gov. For instance, a breast cancer survivor should pay attention to any new swelling or heaviness in the hand, arm, or chest (on the treated side), even months or years post-mastectomy. Similarly, someone who had lymph nodes removed in the groin for pelvic cancer should watch for one leg becoming larger than the other. Recognizing these early symptoms of lymphedema and reporting them to your doctor promptly is critical cancer.govcancer.gov. Early-stage lymphedema can often be managed with conservative measures to reduce swelling and prevent permanent damage, whereas long-standing lymphedema can lead to more severe fibrosis and complications.
Why Early Precautions Are Critical
Taking precautions at the first hint of lymphedema can make a life-changing difference. In the early stages, the swelling is mostly fluid and can be minimized or even reversed with proper care. However, if lymphedema is left unchecked, that stagnant fluid triggers inflammation and fat deposition in the tissues, leading to irreversible changes like scar tissue, hardened skin, and further blockage of lymph flow cancer.gov. Advanced lymphedema (stages 3–4) can cause a massively enlarged limb (elephantiasis) with recurrent infections and mobility issues – a condition that has no cure short of surgery.
By contrast, early intervention and precautions help break this vicious cycle. The goal is to keep mild swelling from progressing: if you start using compression garments or lymphatic exercises when swelling is minimal, you can often reduce fluid buildup and prevent tissue damage. Studies have shown that patients who get educated and treated early have better outcomes and fewer complications than those who wait. In short, preventing lymphedema from worsening is far easier than treating advanced lymphedema, so don’t hesitate to act on early warning signs.
Moreover, early precautions are vital to avoid infections. Even mild lymphedema can compromise your immune defenses in that limb – fluid stagnation and skin breaks allow bacteria to thrive, leading to cellulitis (a serious skin infection) that in turn makes swelling worse cancer.gov. Each infection can damage lymphatic vessels further. Thus, by diligently protecting your skin and addressing swelling early, you reduce the risk of a dangerous infection and the subsequent spike in lymphedema that often follows cancer.govcancer.gov.
Remember: Lymphedema may be a chronic condition, but early and continuous management can keep it well-controlled. Next, we’ll outline practical, patient-focused precautions to help prevent lymphedema progression and safeguard your health.
Practical Precautions to Prevent Lymphedema Progression
Whether you are at risk for lymphedema (after cancer surgery) or already have mild swelling, these precautions can help prevent progression and protect your limb for the long term. Incorporate these patient-focused tips into your daily life:
-
Maintain diligent skin care and hygiene: Keep the skin of the affected limb clean and moisturized every day to prevent dryness and cracks. Gently wash and dry the skin, and use a fragrance-free lotion to keep it supple. Take care of your nails (no cutting cuticles) to avoid openings in the skin. Even small cuts or fungal infections can invite bacteria. Treat any cut, scrape, or insect bite immediately – wash with soap and water, apply an antiseptic and bandage it. Good skin hygiene lowers the risk of cellulitis and skin breakdown in the swollen limb.
-
Protect the limb from injury and infection: Because trauma can trigger or worsen lymphedema, be vigilant about preventing injuries. Avoid needle sticks or blood pressure cuffs on the at-risk arm – use the other arm for blood draws, IVs, injections, and BP measurements. Wear gloves when gardening, doing housework with chemicals, or handling pets to prevent bites, scratches, and harsh irritants on your skin. Use insect repellent to avoid bug bites, and apply sunscreen to avoid sunburn on the affected area, since sunburn can increase swelling. Even seemingly minor traumas (a pinch, burn, or cut) can lead to inflammation that overloads your lymph system, so take precautions to pamper and protect that limb.
-
Avoid tight clothing and jewelry: Do not wear anything that constricts the affected arm or leg, such as tight sleeves, rings, bracelets, or elastic bands, as these can impede lymphatic drainage. Opt for loose-fitting clothes and consider padding pressure points (like under bra straps) if needed. When possible, carry handbags, purses, or heavy packages with your unaffected arm to avoid putting extra pressure on the shoulder or arm at risk. Even a blood pressure cuff squeezing the arm can cause issues, so politely remind healthcare providers to use the other limb.
-
Use compression garments as prescribed: Wearing a properly fitted compression sleeve or stocking is a cornerstone of lymphedema prevention and management. The gentle external pressure helps prevent lymph fluid from pooling in the limb. If your doctor or lymphedema therapist recommends compression, get professionally measured for a garment that fits your limb’s dimensions. A well-fitted compression sleeve can significantly reduce swelling during daily activities or travel. (Tip: If you plan to fly on an airplane or do prolonged sitting/standing, wearing your compression garment can offset pressure changes and gravity effects.) Always ensure proper fit – an ill-fitting or overly tight garment can worsen lymphedema, so consult your healthcare team on the right size and type.
-
Keep the limb moving with gentle exercise: Regular light exercise and muscle activity help stimulate lymph flow and improve drainage. For example, if you have arm lymphedema, simple range-of-motion exercises, light arm pumps, and squeezing a stress ball can activate muscle pumps to move fluid. Walking, swimming, or yoga are often excellent for leg lymphedema. Always consult your doctor or physical therapist about safe exercises for your condition – they can provide a tailored exercise plan. Avoid strenuous, repetitive motions or heavy lifting with the affected limb, especially in the early postoperative period. Activities like vigorous scrubbing, weight training without guidance, or carrying very heavy objects with that limb could strain the compromised lymphatics. The key is staying active without overexertion. Exercise also helps with weight control, which is important because being overweight increases lymphatic load and lymphedema risk cancer.gov. Maintain a healthy weight through diet and physical activity as part of your lymphedema care.
-
Elevate the limb whenever possible: Taking breaks to elevate the affected arm or leg above heart level can significantly reduce swelling. Elevation lets gravity help drain fluid out of the limb. For instance, propping your arm up on pillows while resting, or using a recliner for leg elevation, can ease that heavy feeling. Aim to elevate a few times a day, especially after exertion. Even during sleep, some patients find it helpful to keep the limb slightly raised on a pillow. Elevation is most effective in early-stage lymphedema where fluid is still movable and not yet fibrous.
-
Be cautious with temperature extremes: Avoid exposing the affected limb to extreme heat or cold, as this can aggravate swelling. Heat causes blood vessels to dilate and can increase fluid leakage, while extreme cold can reduce circulation and damage the skin. That means no hot tubs or saunas, and skip very hot baths for that limb. Do not apply heating pads or very hot packs on the swollen area. If using ice packs for soreness, wrap them in a cloth and limit the time – never apply ice directly for long periods on a lymphedematous limbh. In hot weather, keep the limb cool; in winter, prevent chapping by keeping it warm and moisturized. Basically, moderation is key – protect the limb from temperature extremes to avoid sudden changes in circulation.
-
Monitor and respond to any changes: Perhaps most importantly, stay alert to your limb’s condition day to day. If you notice any sign of infection – such as redness, warmth, sudden swelling, or fever – contact your doctor right away. Even a mild infection can escalate with lymphedema, so prompt treatment (often with antibiotics) is critical. Likewise, if swelling seems to be increasing or the limb feels harder, schedule a check-up. Sometimes a short course of physical therapy or adjustment in compression can get you back on track. Never ignore worsening symptoms, and keep all follow-up appointments with your lymphedema therapist or surgeon. Vigilant self-monitoring, along with these precautions, will give you the best chance of preventing arm swelling after cancer surgery or stopping early lymphedema from progressing further.
By following the above precautions, many patients manage to avoid serious lymphedema or keep it in a mild, manageable state. Of course, prevention and conservative care are the first lines of defense. In the next section, we discuss advanced treatments available – because even if lymphedema becomes chronic, modern lymphedema management in Lucknow offers new hope through innovative surgical options.
Lymphedema Management in Lucknow: Advanced Surgical Options at Kayakriti
For some patients, despite precautions and therapy, lymphedema can be persistent or significantly affect quality of life. The swelling might remain or progress over time (especially in moderate to advanced cases). In such situations, specialized surgical interventions can help restore lymphatic circulation and reduce the burden of swelling. As a leading lymphedema surgeon in Lucknow, Dr. Amit Agarwal offers cutting-edge microsurgical treatments at Kayakriti Plastic Surgery to improve outcomes for patients with chronic or post-cancer lymphedema. Two advanced options in lymphedema surgery are Lymphovenous Bypass (LVB) and Vascularized Lymph Node Transfer (VLNT), which can be done alone or in combination depending on the case. Below we explain these techniques:
Lymphovenous Bypass (LVB / Lymphaticovenular Anastomosis)
Lymphovenous bypass (LVB) is a minimally invasive microsurgery that reroutes the lymph flow around damaged areas. In this procedure, the surgeon connects tiny lymphatic vessels directly into nearby venules (small veins) so that lymph fluid can drain into the bloodstream, bypassing the blocked lymph nodes. These lymphatic–venous connections, also called lymphaticovenular anastomoses, act like new “detours” or drainage pathways for the excess lymph. The operation is typically done through a few small incisions and can often be performed as an outpatient procedure.
LVB is generally considered first-line among surgical approaches because it is relatively safe and effective for early-stage lymphedema. By restoring some lymphatic drainage, it can significantly reduce swelling – clinical studies report an average limb volume reduction of about 20–30% at one year post-surgery with successful LVB. Many patients also experience fewer episodes of swelling and may not need to use compression as frequently after healing. Dr. Agarwal uses supermicrosurgical techniques under high magnification to identify functioning lymphatics and veins to connect. Over time, the new lymphatic-venous channels help to continually shunt fluid away from the limb, improving symptoms and potentially slowing further progression of lymphedema.
Vascularized Lymph Node Transfer (VLNT)
Vascularized lymph node transfer (VLNT) is a more complex reconstructive surgery for lymphedema, usually reserved for moderate to advanced cases or when lymphatic vessels are severely damaged. VLNT involves transplanting healthy lymph nodes (along with their blood supply) from one part of the body to the affected area. Common donor sites for lymph nodes include the lower abdomen (omental nodes), groin, neck, or axilla of the opposite side – Dr. Agarwal carefully selects a donor site that can spare a couple of lymph nodes with minimal risk to that area. In the procedure, a small cluster of lymph nodes and surrounding tissue is microsurgically removed from the donor site and then grafted into the lymphedematous limb, typically near the area of blockage. The arteries and veins of the node flap are connected to blood vessels in the recipient limb so that the transferred nodes have a live blood supply and can function in their new location.
Over the following months, the transplanted lymph nodes can gradually create new lymphatic connections and start absorbing excess fluid in the swollen limb. VLNT essentially tries to “seed” the affected area with fresh lymphatic tissue to rebuild drainage pathways. It is a more invasive surgery than LVB and may require a short hospital stay. However, VLNT can be very beneficial, especially if LVB alone is not sufficient or if there are no usable lymphatic channels to bypass (such as in longstanding lymphedema). Studies have shown notable improvements after VLNT: limb circumference and heaviness often decrease, patients report reduced discomfort, and importantly the incidence of infections (cellulitis) drops dramatically. In one long-term study, about 42% of patients were able to discontinue use of compression garments after VLNT, and cellulitis episodes were reduced tenfold. These outcomes underscore how restoring lymphatic function can improve not just swelling, but overall health and quality of life for lymphedema patients.
At Kayakriti, Dr. Amit Agarwal employs both LVB and VLNT as part of a comprehensive approach to lymphedema. Each patient undergoes a thorough evaluation (including imaging of lymphatics when needed) to determine the best treatment plan. In some cases, combined therapy is used – for example, performing a lymph node transfer and adding a few lymphovenous bypass connections to maximize drainage. These microsurgical treatments are cutting-edge techniques in the field of lymphology, and Dr. Agarwal’s advanced training in microvascular surgery allows him to perform them with precision. The goal of surgical intervention is to reduce swelling, soften the hardened tissues, decrease dependence on compression garments, and prevent recurrent infections, thereby improving limb function. While no procedure can guarantee a full “cure” of lymphedema, many patients experience meaningful relief and can resume activities that swelling previously hindered. Modern lymphedema surgery offers hope for those suffering from chronic post-cancer swelling and can be especially life-changing for patients who had lost confidence due to a heavy, enlarged limb.
(Note: Not every lymphedema patient is a candidate for surgery – these procedures are typically considered in moderate Stage II or III cases that don’t fully respond to conservative management. An evaluation with a lymphedema specialist is necessary to determine the appropriate interventions for your situation.)
Living with Lymphedema: Long-Term Management and Quality of Life
Lymphedema is a chronic condition, but with the right management plan, you can lead a healthy and active life. Education, lifestyle adjustments, and regular medical follow-up are the cornerstones of long-term control. It’s important to understand that while lymphedema can be managed very well, it doesn’t simply “go away” – even after surgical treatment, ongoing care and precautions remain important because there is no absolute cure yet. Here are some key points for thriving with lymphedema over the long term:
-
Stick to your routine: Consistency in wearing compression garments (as directed), doing daily lymphatic exercises or self-massage (if taught by your therapist), and protecting your limb will yield the best results. Skipping these measures for extended periods could allow swelling to return. Most patients find that once they incorporate these habits, it becomes a seamless part of their day – much like brushing your teeth.
-
Regular medical check-ups: Stay in contact with your healthcare team. Schedule periodic visits with your surgeon or lymphedema therapist to monitor your limb’s status. They can measure your limb, adjust compression levels, and update your exercise plan as needed. If you’ve had surgery like LVB or VLNT, follow-up is essential to track improvements over months and address any issues. Don’t hesitate to reach out sooner if you notice changes; early intervention can often nip problems in the bud.
-
Healthy lifestyle: Focus on overall health, as it directly impacts lymphedema. Keeping your weight in a healthy range can reduce stress on your lymphatic systemcancer.gov. Eat a balanced diet low in salt (excess sodium can cause fluid retention). Stay hydrated and avoid excessive alcohol (which can dehydrate and thicken lymph fluid). Regular aerobic exercise like walking, swimming, or cycling is excellent for circulation – just be sure to wear compression during exercise if advised, and gradually build up intensity with guidance. Many lymphedema patients successfully participate in activities like yoga, Pilates, or light weight training; these can improve mobility and mood, which is great for long-term wellness.
-
Emotional well-being and support: It’s normal to feel frustrated or self-conscious about lymphedema at times. Seek support if you need it – connect with lymphedema support groups (there are patient communities both locally and online), or talk to a counselor if the stress is impacting you. Sometimes just discussing with others who understand can be a huge relief. Remember that you are not alone, and lymphedema does not define you. By taking control of your care, you’re empowering yourself, and that confidence can greatly improve your quality of life.
-
Quality of life focus: Modern lymphedema care is all about improving your daily experience. That means not only reducing swelling, but also addressing pain, improving limb function, and enabling you to do the things you enjoy. For example, if flare-ups of swelling are making it hard to cook, garden, or play with your kids, let your provider know – sometimes a change in compression knit or adding a physical therapy session can help you get back to those activities comfortably. Many patients find that once their lymphedema is well-managed, they forget about it for most of the day and can truly live normally, aside from a few extra precautions. This is our ultimate goal: to ensure lymphedema has minimal impact on your lifestyle, longevity, and happiness.
In summary, lymphedema requires mindful management, but it should not stop you from enjoying life’s precious moments. By staying proactive with care – and leveraging medical advances when needed – you can control lymphedema rather than letting it control you.
Take Action: Get Expert Lymphedema Help in Lucknow
If you or a loved one is dealing with lymphedema or post-mastectomy arm swelling, don’t wait for things to worsen. Early consultation and treatment can make a huge difference. Kayakriti Plastic Surgery in Lucknow is here to support you with comprehensive lymphedema care. Led by Dr. Amit Agarwal (American Board-Certified plastic surgeon and microsurgery expert), our team provides patient-centric guidance – from preventive education and therapy to cutting-edge surgeries like lymphovenous bypass and lymph node transfer. We understand the physical and emotional challenges of lymphedema and are committed to helping you protect your health and quality of life every step of the way.
Take the first step towards relief today – call us at 9695940009 or visit our website to schedule a consultation. Let us partner with you in preventing lymphedema progression, restoring comfort, and reclaiming the active life you love. Remember, with the right precautions and expert care, you are in control of your lymphedema journey!